
AI, is to think positive
Summary
Social Accountability of medical schools is facing delays in turning from the conceptual phase into real day to day work of medical schools. One of the reasons for this delay is the lack of training of faculty members on how to move towards social accountability. This article aims to introduce the Appreciative Model Approach with its 5D-model as a feasible and positive change initiative to be used by faculty members and school leadership to move social accountability forward.
Article
In 1995, the World Health Organization (WHO) announced the definition of social accountability of medical schools (Boelen and Heck 1995). The WHO document described social accountability in the field of medical education as the obligation of the medical schools to conduct their functions -- education, service, and research -- to address the priority health concerns of the society they serve; this society extends from the local community to the whole nation (Boelen and Heck 1995)(GCSA 2010). One the important dimensions included in the WHO description is that all stakeholders, including society members, should participate in defining the priority concerns that will govern the medical school's activities (Boelen and Heck 1995)(Boelen 1999).
Since the announcement of the definition, many initiatives have been implemented to put social accountability into action; they are crowned in the year 2010 by the publication of the Global Consensus for Social Accountability of Medical Schools that described the way forward towards social accountability through 10 strategic directions (GCSA 2010). Other initiatives include, but are not limited to, the Tunis Declaration (The Network:TUFH 2017), the National Health Workforce Accounts, and Dublin Declaration adopted by the HRH Forum (WHO 2017).
Despite all the described initiatives, still, the implementation of social accountability on the ground into the daily activities of medical schools is not as expected (Abdalla, Boelen, and Osman 2019). One of the reasons described is the lack of training of faculty members in the schools on the practical tips and steps of how to change and run social accountability activities (Abdalla, Boelen, and Osman 2019).
This article aims to fill the gap through empowering faculty members and concerned personnel and stakeholders in medical schools to acquire practical tips and skills on leading change towards social accountability using the Appreciative Inquiry (AI) Model of transformation. The AI Model is unique because it builds on the strengths and positives and the ordinary problem-solving approach of “what is going wrong and what needs to be changed” (Sandars and Murdoch-Eaton 2017); in the SA, the AI transformation will make the base of change on the existing successes related to the medical school-society relationship.
The AI approach requires a mindset change in medical schools, starting from the way the questions will be asked, the difference from “what things do we need to change to be socially accountable?” to “what strengths do we have and can we build on to be socially accountable?” with aim to motivate personnel and mobilize resources to change the situation in medical schools along the continuum of social accountability (Sandars and Murdoch-Eaton 2017).
The AI process is based on five steps (5D-model); Definition, Discovery, Dream, Design, and Delivery (Delgadillo, Palmer, and Goetz 2016)(Sandars and Murdoch-Eaton 2017), as illustrated in Figure 1 below.
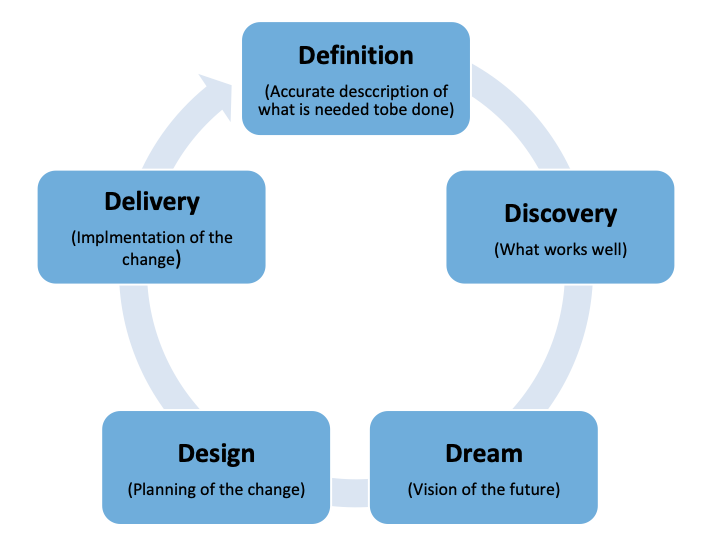
Figure 1: The 5D-model of the appreciative inquiry (AI) approach
The successful implementation of the 5D-model depends on the ability to raise the suitable, answerable questions for each of the D’s, the collective answers of these items will ease the change process (Sandars and Murdoch-Eaton 2017). Below we are going to explain the meaning and the use of each of the five D’s concerning social accountability of medical schools (Sandars and Murdoch-Eaton 2017; Delgadillo, Palmer, and Goetz 2016):
➢ Definition: This step is meant for the accurate description of what is needed to be done for that particular change process; clear topic/area of work definition helps to formulate the questions -- in the other steps -- necessary to find what you want to do. It may be beneficial at this stage to define who is going to do it. The questions that may raise at this stage may be:
- What action do we need to do in the education part to be more socially accountable?
- What action do we need to do in the service part to be more socially accountable?
- What action do we need to do in the research part to be more socially accountable?
- What change in the mission do we need to do to reflect social accountability?
- Who is the suitable personnel in the college can take responsibility for this change?
Discovery: This step is meant to use the appreciative eye to identify the processes that work well, and to determine the actual best practices in the institutes that relate to the targeted topic or area of change identified in the first step. For example, if the area of change is social accountability in the education function of the medical school, then the following can be examples of questions that may need to be answered:
- What part of our mission obligates us to have a curriculum that addresses the health problems in society?
- What is the classification of our curriculum, is it community-oriented or community-based curriculum?
- What is good about what we are doing in the community-based activities in the curriculum? What achievements?
- What is the part of the curriculum that addresses the health problems in society?
- How did we define the health problems to be included in the curriculum? What is the role of society in that?
Dream: This step is for the vision of the future: what the current situation of the social contract and commitment could be like in the future when the institute is more socially accountable. This step is crucial as it will determine actions in the following phases. Below are some of the questions that may be asked:
- What might the curriculum be like when considering the priority health problems?
- What would the achievement be if we were more socially accountable than we are?
- What would the ideal future socially accountable curriculum be like?
➢ Design: This stage is for planning and prioritizing processes that would work/achieve the dreams that were agreed upon by completing the phase above. At this stage, examples of questions that may need to be answered are:
- What needs to be done differently to achieve your chosen future situation?
- What resources are required, or who can help you, to fulfill your chosen future situation?
- What do we need to do to realize that future?
Delivery: This is the phase of implementation of the proposed actions in the design phase. By the end of this phase, the change should have been on the ground, sustainable, and ready for evaluation. Examples of questions to be answered at this phase are:
- How can we sustain the changes in the curriculum we are doing?
- What needs to be done to ensure the continuity of the changes?
- What model of curriculum development will we follow?
- What resources do we need to avail to make the change happened?
In conclusion, the appreciative inquiry approach can be a suitable model for change towards more social accountability in medical schools as it builds on the strength of what the institute is doing, this may ease the change process and decrease the resistance of change. AI is a feasible and positive form of change model that avoids deficit-based solutions that are associated with defensiveness (McIntosh, Freeth, and Berridge 2013)(Rama, Falco, and Balmer 2018).
Works Cited
Abdalla, M. E., Charles Boelen, and Wail N. Osman. 2019. “Development and Evaluation of an Online Course about the Social Accountability of Medical Schools.” Journal of Taibah University Medical Sciences 14 (3): 241–45. https://doi.org/10.1016/j.jtumed.2019.03.004.
Boelen, C. 1999. “Adapting the Health Care Institutions and Medical Schools to Societies Needs.” Academic Medicine 74 (8 Supplement): S11–20.
Boelen, C, and J Heck. 1995. “Defining and Measuring the Social Accountability of Medical Schools.” Geneva, Switzerland: Division of Development of Human Resources for Health. https://apps.who.int/iris/handle/10665/59441.
Delgadillo, L.M., L. Palmer, and J. Goetz. 2016. “A Case Study Demonstrating the Use of Appreciative Inquiry in a Financial Coaching Program.” Family and Consumer Sciences Research Journal 45 (2): 166–78.
GCSA. 2010. “Global Consensus for Social Accountability of Medical Schools.” Global Consensus for Social Accountability of Medical Schools. 2010. healthsocialaccountability.sites.olt.ubc.ca/files/2011/06/
McIntosh, Paul, Della Freeth, and Emma Jane Berridge. 2013. “Supporting Accomplished Facilitation: Examining the Use of Appreciative Inquiry to Inform the Development of Learning Resources for Medical Educators.” Educational Action Research 21 (3): 376–91. https://doi.org/10.1080/09650792.2013.815044.
Rama, Jennifer A., Carla Falco, and Dorene F. Balmer. 2018. “Using Appreciative Inquiry to Inform Program Evaluation in Graduate Medical Education.” Journal of Graduate Medical Education 10 (5): 587–90. https://doi.org/10.4300/JGME-D-18-00043.1.
Sandars, John, and Deborah Murdoch-Eaton. 2017. “Appreciative Inquiry in Medical Education.” Medical Teacher 39 (2): 123–27. https://doi.org/10.1080/0142159X.2017.1245852.
The Network:TUFH. 2017. “Tunis Declaration.” 2017. thenetworktufh.org/wp-content/uploads/.
WHO. 2017. “National Health Workforce Accounts – A Handbook.” 2017.
Author bio

Dr. Mohamed Elhassan is an Assistant Professor of Medical Education at the College of Medicine at the University of Sharjah, United Arab Emirates; Fellow of the Academy of Medical Educator; Acting Director of Medical Education Center at the University of Sharjah, United Arab Emirates; member of the International Reference Group on Social Accountability of Medical Schools; and member of the Society of Cost and Value in Health Professions Education. He also is a member of the Network-TUFH and Social Accountability and Accreditation working group, the Network-TUFH. Dr. Elhassan’s research Interests include social accountability of health profession education, accreditation of health professions education, and cost and value of health professions education.


